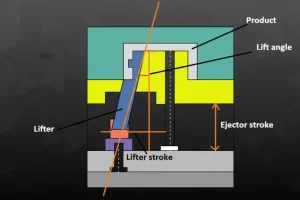
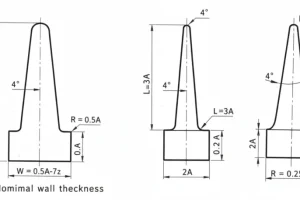
Medical device moulage par injection La certification ISO 13485¹ ne consiste pas simplement en une fabrication ordinaire avec des documents supplémentaires—c'est une approche complètement différente de la gestion de la qualité. Après deux décennies de production de composants médicaux, j'ai vu des fabricants se débattre avec la transition de l'ISO 9001 vers le monde des dispositifs médicaux. La différence ne se limite pas à des exigences plus strictes ; c'est un changement fondamental dans la manière de penser le risque, la traçabilité et le contrôle des processus.
- L'ISO 13485 exige une réflexion basée sur les risques tout au long du processus de moulage par injection
- Les environnements de salle blanche et le contrôle de la contamination sont obligatoires pour la fabrication de la plupart des dispositifs médicaux
- La validation des processus via les protocoles IQ, OQ et PQ est essentielle pour l'approbation réglementaire
- Une traçabilité complète de la matière brute au dispositif fini doit être maintenue
- La sélection des matériaux nécessite des tests de biocompatibilité et une documentation de conformité réglementaire
Qu'est-ce que l'ISO 13485 et en quoi diffère-t-elle de l'ISO 9001 ?
L'ISO 13485 et ses différences avec l'ISO 9001 sont définies par la fonction, les contraintes et les compromis expliqués dans cette section. Pour une vision plus large de conception de moules d'injection, our pillar guide covers tooling structure, thermal control, and manufacturability tradeoffs.
L'ISO 13485¹ est la norme de gestion de la qualité spécifiquement conçue pour les fabricants de dispositifs médicaux. Bien qu'elle partage certaines caractéristiques avec l'ISO 9001, les similitudes s'arrêtent rapidement. L'ISO 13485 supprime l'exigence d'« amélioration continue » de l'ISO 9001 en faveur de « maintenir l'efficacité »—car dans les dispositifs médicaux, des changements non autorisés peuvent tuer des personnes. La norme exige une intégration de la gestion des risques, une conformité réglementaire et une surveillance post-marketing qui va bien au-delà des systèmes de qualité générale.
Les implications pour le moulage par injection sont significatives. Alors que l'ISO 9001 pourrait accepter des améliorations de processus basées sur des gains d'efficacité, l'ISO 13485 exige un contrôle formel des changements, une évaluation des impacts et souvent une notification réglementaire pour toute modification de processus. Chaque paramètre de moulage par injection—température, pression, durée du cycle—devient partie d'un processus validé qui ne peut être ajusté de manière arbitraire. Un document étape du processus de moulage par injection la carte permet de maintenir chaque paramètre lié au même dossier de preuves utilisé lors de la validation.
| Aspect | ISO 9001 | ISO 13485 |
|---|---|---|
| Focus principal | Satisfaction du client | Sécurité et efficacité |
| Philosophie d'amélioration | Amélioration continue | Maintenir l'efficacité |
| Risk Management | Considération facultative | Intégration obligatoire |
| Conformité réglementaire | Non spécifié | Exigence explicite |
| Changements de processus | Encouragé si bénéfique | Contrôlé et validé |
| Niveau de documentation | Modéré | Extensive et traçable |
| Activités post-livraison | Retour client | Surveillance post-commercialisation |
« Les installations de moulage par injection certifiées ISO 13485 doivent maintenir des processus validés qui ne peuvent être modifiés sans approbation formelle. »Vrai
C'est absolument correct. L'ISO 13485 exige que tous les processus de fabrication soient validés et contrôlés. Tout changement des paramètres de moulage par injection, des matériaux ou des procédures doit passer par un processus de contrôle formel des changements avec évaluation des risques et validation. Cela garantit que les modifications ne compromettent pas la sécurité ou l'efficacité du dispositif.
« L'ISO 13485 n'est que l'ISO 9001 avec des exigences documentaires supplémentaires pour les dispositifs médicaux. »Faux
Il s'agit d'une simplification dangereuse. Bien que l'ISO 13485 utilise l'ISO 9001 comme fondement, elle modifie fondamentalement l'approche de la gestion de la qualité. Le passage de l'amélioration continue au maintien de l'efficacité, l'intégration obligatoire de la gestion des risques et les exigences de conformité réglementaire représentent une philosophie de la qualité complètement différente, et pas seulement des documents supplémentaires.
Quelles exigences en matière de salle blanche s'appliquent au moulage par injection médical ?
Cette section traite des exigences de salle blanche applicables au moulage par injection médical et de leur impact sur le coût, la qualité, les délais ou le risque d'approvisionnement. Les exigences de salle blanche pour le moulage par injection médical dépendent de la classification du dispositif et du risque de contamination. Les dispositifs de classe I peuvent n'avoir besoin que de contrôles de propreté de base, tandis que les dispositifs implantables nécessitent des environnements de classe ISO 14644-1 de niveau 7 ou supérieur. Le défi n'est pas seulement de maintenir la salle blanche, c'est d'intégrer l'équipement de moulage par injection dans des environnements contrôlés sans compromettre ni la propreté ni le processus de moulage.
Le contrôle de la température devient critique lorsque votre système CVC de salle blanche entre en conflit avec les exigences thermiques du moulage par injection. Nous avons vu des installations lutter pour maintenir un contrôle de température de ±2°C tout en faisant fonctionner des machines de 1850 tonnes qui génèrent d'énormes charges thermiques. Les schémas de flux d'air doivent être conçus autour du placement des machines, et les schémas de flux du personnel nécessitent une attention particulière, surtout lors des changements de moule qui peuvent prendre 2 à 3 heures.
| Classe salle blanche | Particules ≥0,5μm par m³ | Applications des dispositifs médicaux | Exigences typiques |
|---|---|---|---|
| ISO 5 | 3,520 | Dispositifs implantables, composants stériles | Blouse complète, flux laminaire |
| ISO 6 | 35,200 | Instruments chirurgicaux critiques | Cleanroom suits, controlled access |
| ISO 7 | 352,000 | Non-sterile implants, diagnostic devices | Lab coats, shoe covers |
| ISO 8 | 3,520,000 | External medical devices | Basic protective clothing |
| Standard Room | >3,520,000 | Class I devices (low risk) | Good housekeeping practices |

Comment la validation des processus (IQ, OQ, PQ) est-elle exécutée dans le moulage médical ?
This section is about Validation des processus1 (iq, oq, pq) executed in medical molding and its impact on cost, quality, timing, or sourcing risk. Process Validation IQ/OQ/PQ in medical injection molding follows the protocol that proves your process consistently produces parts meeting specifications. Installation Qualification (IQ) verifies equipment installation according to specifications—checking that your injection molding machine can actually reach the temperatures and pressures specified in your process. This is not a quick check; expect 2-3 days of documentation and testing per machine.
Operational Qualification (OQ) proves the equipment performs as intended across its operating ranges. For injection molding, this means testing temperature uniformity across heating zones, pressure accuracy, and repeatability. You’ll run test cycles at minimum, maximum, and typical operating parameters. Performance Qualification (PQ) is where you prove the entire process produces acceptable parts—typically requiring 30 consecutive successful production runs with full dimensional and functional testing.
The documentation burden is substantial. Each validation protocol can generate 200-500 pages of documentation, and any equipment modifications require revalidation. We maintain separate validation packages for each mold and material combination because the FDA considers these different processes. The investment is significant—budget USD 15,000-30,000 and 4-6 weeks per process validation depending on complexity, and align the validation calendar with realistic Temps de production du moulage par injection before promising launch dates.
“Process validation must be completed before commercial production of medical devices can begin.”Vrai
This is correct and non-negotiable. FDA regulations and ISO 13485 requirements mandate that processes be validated before commercial production. You cannot ship medical devices produced on unvalidated processes. This includes injection molding parameters, environmental controls, and quality control procedures. Any process changes require revalidation before resuming production.
“Once a process is validated, it never needs revalidation unless equipment breaks down.”Faux
This is incorrect and potentially dangerous. Revalidation is required for equipment modifications, process parameter changes, facility moves, personnel changes affecting process control, and periodic revalidation (typically annually or biannually). Even software updates on injection molding machine controllers can trigger revalidation requirements.
Quel rôle joue la traçabilité dans la conformité à l'ISO 13485 ?
This section is about role does traceability play in iso 13485 compliance and its impact on cost, quality, timing, or sourcing risk. Traceability in ISO 13485 medical injection molding means you can track every component from raw material lot to the specific patient who received the device. This isn’t just batch records—it’s complete genealogy including material lot numbers, processing parameters, quality test results, and personnel involved. When a medical device fails in the field, regulators expect you to identify every potentially affected device within hours, not days.
The injection molding implications are extensive. Every material lot must be segregated and tracked through processing. Regrind usage requires documentation showing contamination ratios and approval records. Machine maintenance records become part of device history because a worn screw or contaminated barrel could affect product quality. We maintain Device History Records⁴ (DHR2) that can trace individual parts to specific cavity positions in multi-cavity molds.
Digital systems are practically mandatory for effective traceability. Manual paper systems become unmanageable beyond small production volumes. Expect to invest $50,000-200,000 in MES or ERP systems capable of handling medical device traceability requirements. The system must interface with injection molding machine controls to automatically capture process parameters, and it needs to maintain data integrity for regulatory audits spanning decades.
Quels matériaux sont couramment utilisés dans le moulage par injection médical ?
Medical injection molding materials fall into several categories based on biocompatibility requirements and application. USP Class VI3 materials are the baseline for most medical applications, while implantable devices require ISO 10993 biological evaluation. The most common materials include medical-grade polypropylene, polycarbonate, ABS, and specialty polymers like PEEK for high-performance applications.
Material selection involves more than just mechanical properties. Every material requires biocompatibility documentation, extractables and leachables testing, and often sterilization validation. Polypropylene works well for disposable devices due to gamma and ethylene oxide sterilization compatibility. Polycarbonate offers optical clarity for diagnostic equipment but requires careful processing to avoid stress cracking during sterilization cycles.
Specialty materials command premium pricing but solve specific challenges. PEEK offers chemical resistance and radiolucency for implants but requires processing temperatures above 400°C. Liquid silicone rubber (LSR) provides biocompatibility and flexibility but needs specialized injection molding equipment. Medical-grade materials typically cost 2-5x standard grades, and lot-to-lot certification adds lead time and inventory costs.

Quels sont les avantages et les inconvénients de la conformité à l'ISO 13485 ?
The pros and cons of iso 13485 compliance are the main categories or options explained in this section. ISO 13485 compliance opens doors to lucrative medical device markets but demands significant investment and operational changes. The benefits include access to regulated markets, premium pricing for medical components, and competitive differentiation. However, the compliance burden affects every aspect of operations from documentation requirements to personnel training and process flexibility.
| Aspect | Avantages | Inconvénients |
|---|---|---|
| Market Access | Global medical device markets, regulatory approval | Lengthy certification process, ongoing audits |
| Pricing | Premium rates (20-40% higher), long-term contracts | Higher material and compliance costs |
| Quality Systems | Robust processes, reduced defects, customer confidence | Extensive documentation, slower process changes |
| Competition | Fewer qualified suppliers, market barriers | Higher barriers to entry, specialized expertise required |
| Operations | Systematic approach, risk management integration | Reduced flexibility, longer lead times |
| Investment | Long-term customer relationships, stable revenue | Significant upfront costs, ongoing compliance expenses |
In our Shanghai factory, our team works under ISO 9001, ISO 13485, ISO 14001, and ISO 45001 systems. For medical molding work, 6 machines in a Class M8 dust-free room support cleaner production control, while our broader 47 injection molding machines and 90T to 1850T range keep engineering capacity available for non-medical projects. In our experience across 20+ years of injection molding and tooling, medical projects need documented process validation, material traceability, and in-process checks before a supplier conversation moves from price comparison to qualification.
Comment choisir un partenaire de moulage par injection certifié ISO 13485 ?
Choosing an iso 13485 certified injection molding partner is about tooling capability, quality systems, communication, and commercial fit. Selecting an ISO 13485 injection molding partner requires evaluating capabilities beyond basic certification. Audit their cleanroom facilities, review validation documentation, and assess their regulatory experience. A certificate on the wall doesn’t guarantee competent execution—you need suppliers who understand FDA regulations, EU MDR requirements, and the specific challenges of medical device manufacturing.
Technical capabilities matter as much as certification. Evaluate their injection molding experience with your specific materials and applications. Medical-grade materials often require specialized processing knowledge, and complex geometries may need advanced molding techniques. Review their quality systems, statistical process control capabilities, and documentation practices. A comprehensive sourcing guide can help structure your evaluation process.
Financial stability and scalability are crucial for long-term partnerships. Medical device products often have 10-15 year lifecycles, and you need suppliers who can support growing volumes and regulatory changes. Evaluate their customer base, facility investments, and technical staff retention. The lowest cost supplier rarely survives the compliance demands and investment requirements of sustained medical device manufacturing.
Questions fréquemment posées
How long does ISO 13485 certification take for an injection molding facility?
Initial ISO 13485 certification typically takes 12-18 months for an established injection molding facility with existing quality systems. This timeline includes gap analysis, procedure development, personnel training, system implementation, internal audits, and the two-stage certification audit by a notified body. Facilities starting from scratch—without cleanrooms or validated equipment—should budget 18-24 months. The single biggest delay we see is process validation: each mold-material combination requires its own IQ/OQ/PQ package, and most facilities underestimate this effort. Budget generously and engage an experienced consultant early in the process to avoid costly surprises during the audit phase.
What are the annual costs of maintaining ISO 13485 certification?
Existing injection molding equipment can often be adapted for medical device production, but the path is not straightforward. Equipment must undergo complete Installation Qualification (IQ) to verify it meets specifications, followed by Operational Qualification (OQ) demonstrating capability across operating ranges. Machines need process monitoring and data logging capabilities to capture every shot’s parameters. Cleanroom compatibility is another consideration—hydraulic machines generate heat and particles that can compromise controlled environments. Older machines lacking closed-loop control or adequate documentation interfaces may require significant upgrades (,000-50,000) or replacement. Equipment age alone isn’t disqualifying, but you must prove each machine’s capability through formal qualification protocols.
Can existing injection molding equipment be used for medical device production?
Medical injection molding requires a comprehensive documentation ecosystem. Core documents include Device Master Records (DMR) containing drawings, material specifications, and work instructions; Device History Records (DHR) proving each lot was manufactured per the DMR; process validation protocols and reports (IQ/OQ/PQ); material certifications and biocompatibility test results; equipment qualification and calibration records; standard operating procedures for every process step; and change control documentation for any modifications. Each production lot generates a complete batch record with real-time process parameters, quality inspection results, and full material traceability. Expect documentation volume 10-20x higher than standard injection molding, and plan for digital systems to manage the burden effectively.
What documentation is required for medical injection molding processes?
ISO 13485 fundamentally changes how injection molds are designed, maintained, and modified. Mold designs become controlled documents within the Design Control process—requiring formal design reviews, risk analyses (using tools like FMEA), and documented verification that the mold meets device specifications. Any mold modification, even a seemingly minor cavity polish, triggers a change control process with impact assessment and potential revalidation. Mold maintenance schedules become part of the quality system, with each maintenance event documented in the device history. Multi-cavity molds require cavity-level traceability, meaning each cavity must be identified and tracked individually throughout production. This rigor ensures that mold-related defects can be isolated and corrected without affecting unaffected cavities or devices.
How does ISO 13485 affect injection mold design and manufacturing?
Common sterilization methods for injection molded medical devices include gamma radiation (25-40 kGy), ethylene oxide gas, electron beam, steam autoclave, and hydrogen peroxide plasma. Material selection must account for sterilization compatibility from the design stage: polypropylene and polyethylene tolerate gamma well, but polypropylene can become brittle at higher doses. Polycarbonate may yellow under radiation. PEEK handles virtually all sterilization methods but costs 10-20x standard materials. EtO sterilization requires porous packaging and adequate aeration time to remove residuals. Each device-material-sterilization combination requires its own validation study demonstrating sterility assurance level (SAL) of 10⁻⁶. Failure to validate the specific combination can result in regulatory rejection during device submission.
What sterilization methods are compatible with injection molded medical devices?
ISO 13485 mandates documented training programs for every person whose work affects product quality. Injection molding operators must demonstrate competency in medical device requirements, cleanroom protocols, contamination prevention, and specific process procedures before working independently. Training records must include initial qualification, periodic refresher courses (typically annual), and ad-hoc training for procedure changes or corrective actions. Competency assessments go beyond attendance—operators must demonstrate understanding through practical evaluation. Management retains responsibility for ensuring training effectiveness and maintaining records that survive regulatory audits. Many facilities supplement internal training with external courses on ISO 13485, cleanroom operations, and GMP principles. Budget 40-80 hours of initial training per operator, plus 16-24 hours annually for ongoing requirements.
Are there specific training requirements for personnel in ISO 13485 injection molding?
Yes, ISO 13485 requires documented training for personnel whose work affects product quality. Injection molding operators, process technicians, QC inspectors, warehouse staff, and project engineers managing medical device programs must all receive structured training. This includes initial qualification training, annual refresher courses, and ad-hoc training whenever procedures change or corrective actions are implemented. Training effectiveness must be verified through practical assessment, not just attendance records. Management bears direct responsibility for ensuring competency across all roles. Facilities should budget 40-80 hours of initial training per operator plus 16-24 hours annually for ongoing compliance requirements and continuing education.
Ready to explore ISO 13485 medical device injection molding for your project? Contact ZetarMold to discuss your specific requirements with our certified quality specialists. Our 20+ years of medical device manufacturing experience, combined with comprehensive cleanroom capabilities and validated processes, can help bring your medical device to market safely and efficiently.
-
Process Validation: Process Validation refers to documented evidence that a process, operated within established parameters, can perform effectively and reproducibly to produce a medicinal product meeting its predetermined specifications. ↩
-
DHR: DHR refers to device History Record – compilation of records containing the production history of a finished medical device. ↩
-
USP Class VI: USP Class VI refers to united States Pharmacopeia biological reactivity test standard for plastic materials used in medical devices. ↩